Give patients a voice.
11 March 2021
6.5 min read
By Gareth Kantor.
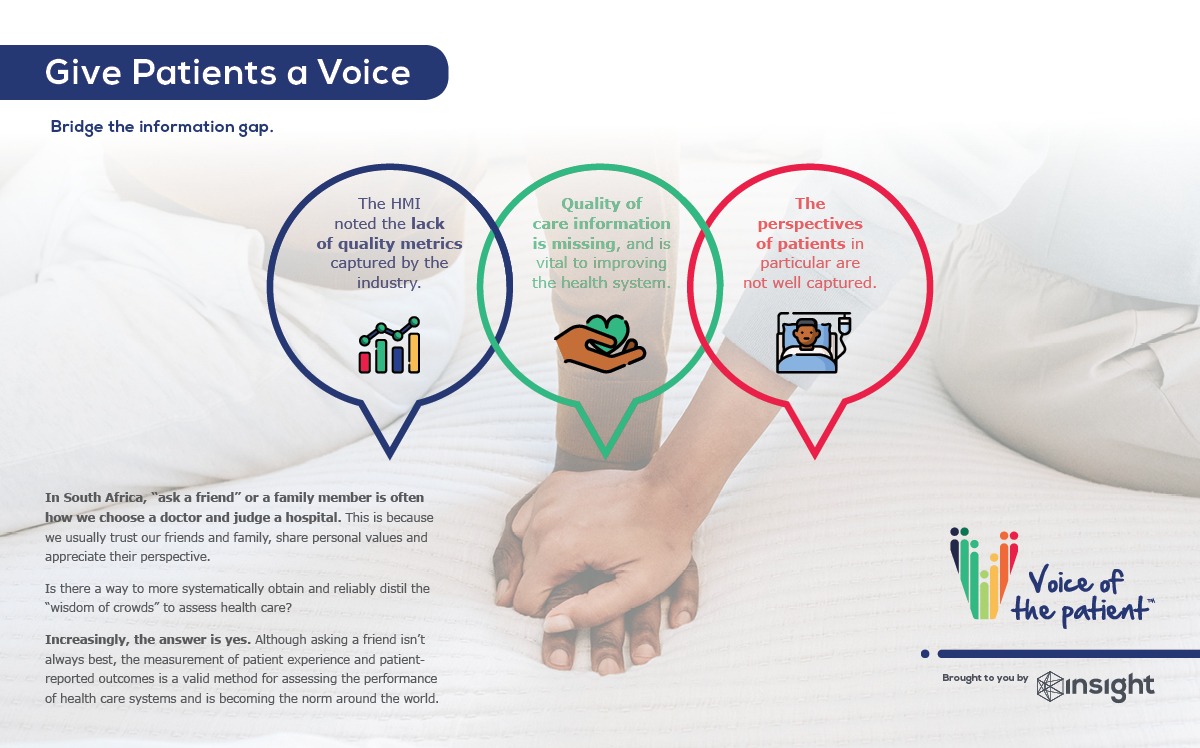
In South Africa, “ask a friend” or a family member is often how we choose a doctor and judge a hospital. This is because we usually trust our friends and family, share personal values and appreciate their perspective.
Is there a way to more systematically obtain and reliably distil the “wisdom of crowds” to assess health care?
Increasingly, the answer is yes. Although asking a friend isn’t always best, the measurement of patient experience and patient-reported outcomes is a valid method for assessing the performance of health care systems and is becoming the norm around the world.
Asking patients doesn’t mean that we drop clinical outcome measures and efficiency metrics, but today, the drive toward patient-centred care goes with the recognition that the best health status and the best health care outcomes are those that patients describe and that they value the most.
Can this wisdom be made available to the health care system, and used responsibly and productively?
The initial approach, 15-20 years ago, resembled consumer reporting on hotels and restaurants. Some of this was done by regulators, or funders. Commercial entities also got involved. But these initiatives often lacked scientific rigor and professional buy-in. Many argued, correctly, that we should not judge health care the same way we assess a burger chain, or a holiday resort.
Instead, assessing health status and health service outcome requires the use of validated measurements that have emerged, grounded in science, endorsed by professional groups.
These are tools for routinely measuring, in a systematic and reproducible way, the reduction of pain and other forms of suffering, the restoration of physical function, improvement in mental health status, health-related quality of life, and other things that patients value. Also, tools to establish whether the delivery of care was respectful, courteous and kind, with continuity, communication and attention to basic needs and comfort.
Don’t professionals do this already?
Health professionals do of course ask patients about their symptoms, their situation, their ability to function; this is, and always has been, a normal part of care. It is not to be replaced by technology. Instead, we can supplement the information available to clinicians at the bedside clinical encounter, collecting it easily and conveniently by electronic means and feeding it back.
With this information in hand, an additional and essential view of the patient and the system becomes available that’s useful in system management, the design of clinical pathways and other key processes and decisions. If available to doctors and patients, it becomes a key new element in clinical decision-making at the patient level.
What will VoP be used for? Improvement and system level decision-making.
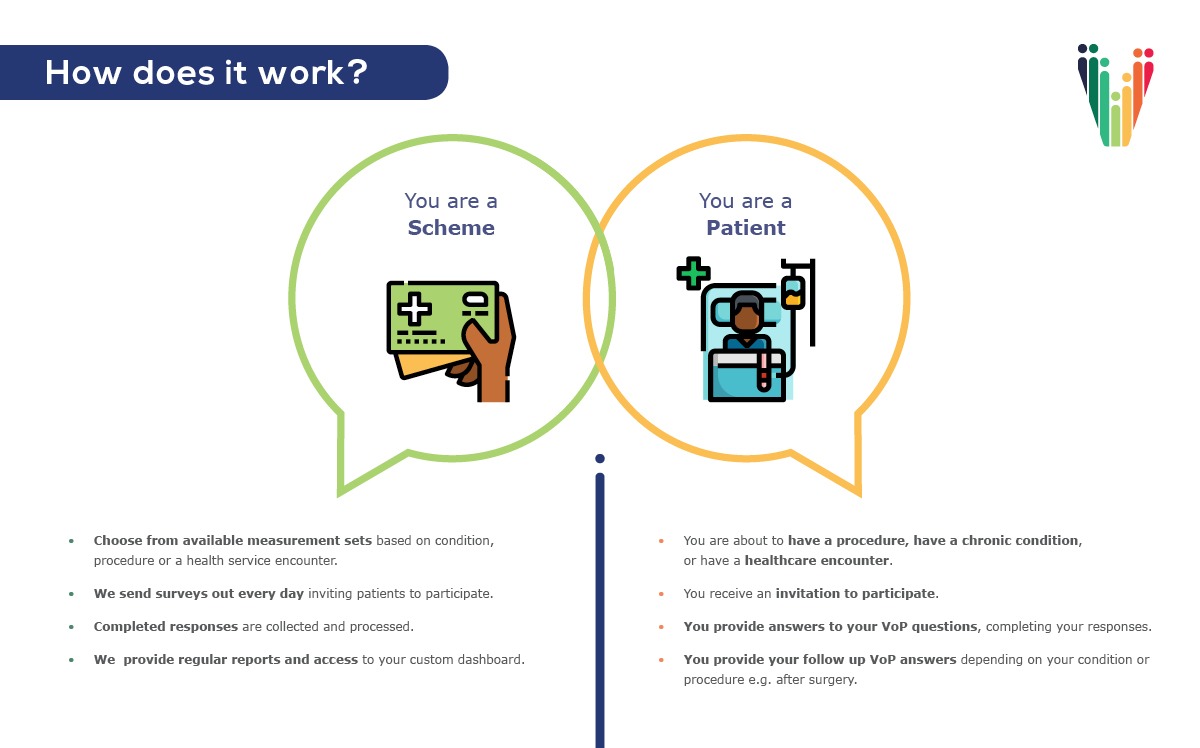
Voice of the Patient has been launched with these aims in mind – to give patients individually and collectively much more of a voice in their care, by scientifically measuring and reporting their experience and outcomes, and making these insights available for assessment and improvement of care.
We’ve begun this work on behalf of clients (medical schemes) by asking patients about their hospital experience and about their experience with primary (GP) care. Measuring the results of elective surgical procedures is another priority. This information is shared, in aggregate, with schemes and depending on arrangements with providers.
What does this mean for health system managers?
Using PREMs (patient-reported experience measures)(e.g. the HCAHPS-based hospital experience survey) and PROMs (patient-reported outcome measures)(e.g. PROMIS, measures from ICHOM, and various condition-specific and quality of life measures) the wisdom of crowds (patients) can help identify variation in outcomes, and in practice. Questions can then be asked – about why this variation occurs and about how the results can be used to design care that is genuinely patient-centred, safer, more effective and an appropriate use of resources.
Overall, these kinds of data correlate quite well with traditional clinical outcomes, also with measures of efficiency. In advanced health systems, such as in Scandinavia, Israel and the US, PREM and PROM data is used to suggest and test ideas for improvement, to help patients understand what to expect from treatment, and to see their progress on treatment over time.
Can it be misused? How can misinterpretation be avoided?
There are always concerns that health care outcome data will be misused or misinterpreted and these must be addressed.
We are aware of the potential for biased population sampling, and for the need, when making comparisons, to “risk adjust”, based on factors like patient age, gender, health status, educational level and socio-economic background. Where comparisons are made, statistical adjustment may be required for differences and challenges that patients bring to each clinical encounter that are not under the control of those from whom they seek care.
Patient participation in Voice of the Patient is always voluntary, and personal health data is protected and private. We will not report individual patient results, only results in aggregate. Individual patient respondents can choose to reveal or share their identity. Outcomes are generally not made available to the public.
VOP operates on behalf of clients and results are for clients (e.g. schemes). Where appropriate, review by professional groups/societies is advised.
Voice of the Patient is a constructive, non-punitive attempt to use the patient voice to improve outcomes for individual patients and families, and for a stronger health system
¹ PROMIS – Patient-Reported Outcomes Measurement Information System – https://www.healthmeasures.net/
² ICHOM – international Consortium for Health Outcomes Measurement – https://www.ichom.org/
VOP’s intention is to offer a means of promoting good patient care, not to find ‘bad apples’, set performance targets, or exclude professionals from networks.
For more information and/or to schedule a discussion about using Voice of the Patient, contact:
Masimba Mareverwa
masimbam@insight.co.za
0836416525
Get an email whenever we publish a new thought piece
The ICHOM 2023 Conference took place in Barcelona this year and was the largest gathering on Value-Based Health Care (VBHC) worldwide. Attended by leading industry experts representing countries from all
2.5 min read
By Insight. "When we die, our bodies become the grass, and the antelope eat the grass. And so we are all connected in the great Circle of Life." – Mufasa
8 min read